Israeli Cannabis Breakthrough Opens New Hope for Fatty Liver Disease
NEW YORK- A new study out of Israel has put Cannabis back into one of the most important conversations in modern medicine: metabolic disease. Researchers at the Hebrew University of Jerusalem have reported that two non-intoxicating Cannabis compounds, CBD and CBG, significantly reduced liver fat and improved metabolic health in experimental models of fatty liver disease. The study, published in the British Journal of Pharmacology, focused on metabolic dysfunction-associated steatotic liver disease, now commonly known as MASLD.
MASLD is the newer medical term for what many people still call non-alcoholic fatty liver disease. It is one of the most common chronic liver conditions in the world and is closely connected to obesity, insulin resistance, type 2 diabetes, high cholesterol, and broader metabolic dysfunction.
That is what makes this research so interesting. This is not another vague claim that Cannabis is “anti-inflammatory” or generally good for wellness. The Israeli team identified specific biological changes in the liver. CBD and CBG appeared to help the liver manage energy stress, reduce harmful fat accumulation, and restore part of the cell’s natural cleanup system.
For Cannabis medicine, that is a much more serious conversation.
Why Fatty Liver Disease Matters
Fatty liver disease starts when excess fat builds up inside liver cells. At first, many people have no obvious symptoms. Over time, however, the condition can progress into inflammation, scarring, cirrhosis, liver failure, and even liver cancer.
It is also a warning sign for wider metabolic trouble. A fatty liver often sits alongside high blood sugar, abdominal weight gain, abnormal cholesterol, and insulin resistance. In many cases, the liver is not the only problem. It is part of a larger breakdown in how the body handles energy, fat, and glucose.
That is why MASLD has become such a major target for drug development. The condition affects a huge percentage of adults globally, yet treatment options remain limited. Doctors still rely heavily on weight loss, diet, exercise, and management of related conditions such as diabetes and high cholesterol.
Those tools matter, but they are not enough for everyone. Many patients struggle to lose enough weight or maintain the lifestyle changes required to reverse the disease. That has created a major need for therapies that can act more directly on liver metabolism.
The breakthrough comes from Israel’s Hebrew University of Jerusalem, where Prof. Joseph “Yossi” Tam, Dr. Liad Hinden, PhD student Radka Kočvarová, and Tam’s research team at the School of Pharmacy in the Faculty of Medicine have been studying how non-intoxicating Cannabis compounds may affect fatty liver disease. Their research found that CBD and CBG significantly reduced liver fat and improved metabolic health in experimental models, pointing to a potential new cannabinoid-based approach to one of the world’s most common chronic liver disorders.
The discovery was led in Israel by Hebrew University of Jerusalem researchers Prof. Joseph “Yossi” Tam, Dr. Liad Hinden, PhD student Radka Kočvarová, and Tam’s team at the School of Pharmacy in the Faculty of Medicine. Their work puts Israeli cannabinoid science at the center of a potentially major advance in metabolic medicine, showing that the non-intoxicating Cannabis compounds CBD and CBG may significantly reduce liver fat and improve metabolic health in experimental models.

Prof. Yossi Tam, front row, second from left, with members of his research lab at the School of Pharmacy at the Faculty of Medicine of the Hebrew University of Jerusalem. (Courtesy/Tom Barnea)
What the Israeli Study Found
The Hebrew University team studied CBD and CBG in a mouse model of diet-induced obesity and fatty liver disease. The animals were fed a high-fat diet, which produced many of the same metabolic problems seen in humans with MASLD, including obesity, impaired glucose control, and excess liver fat.
The mice were then treated with either CBD, CBG, or a control treatment. The researchers looked at body composition, glucose control, blood lipids, liver fat, lipid metabolism, cellular energy markers, and the activity of enzymes involved in clearing cellular waste.
Both CBD and CBG improved key markers of metabolic health. The compounds reduced liver triglycerides, improved blood sugar control, normalized serum lipids, and reduced harmful lipid species associated with metabolic dysfunction.
That alone would be notable. But the more important part of the study was the mechanism.
The researchers found that CBD and CBG increased levels of phosphocreatine and creatine in the liver. Phosphocreatine is best known for its role in muscle, where it helps cells rapidly regenerate energy. In this study, the same energy-buffering system appeared to become more active in the liver.
That suggests the compounds may have helped the liver cope with metabolic stress. A fatty liver is not just a liver with too much fat in it. It is a liver under pressure. Its energy systems are strained, its lipid handling is impaired, and its ability to clear damaging molecules can begin to break down.
CBD and CBG appeared to improve that internal energy resilience.
The Liver’s Cleanup System
The study also found that CBD and CBG helped restore lysosomal function. Lysosomes are the recycling centers of the cell. They break down damaged material, process waste, and help clear unwanted lipid buildup.
In fatty liver disease, that cleanup process can become impaired. Harmful lipid molecules accumulate, including triglycerides and ceramides. Ceramides are especially important because they are linked to insulin resistance, inflammation, and liver injury.
The Israeli researchers found that CBD and CBG reduced triglycerides and ceramides while improving markers connected to lysosomal lipid degradation. In plain English, the compounds appeared to help the liver clean up some of the metabolic mess created by a high-fat diet.
That is a very different story from the usual public discussion around Cannabis.
This is not about getting high. It is not about smoking flower. It is not about using Cannabis as a general lifestyle product. This is about isolated, non-intoxicating cannabinoids being studied as pharmacological tools that may influence liver metabolism in measurable ways.
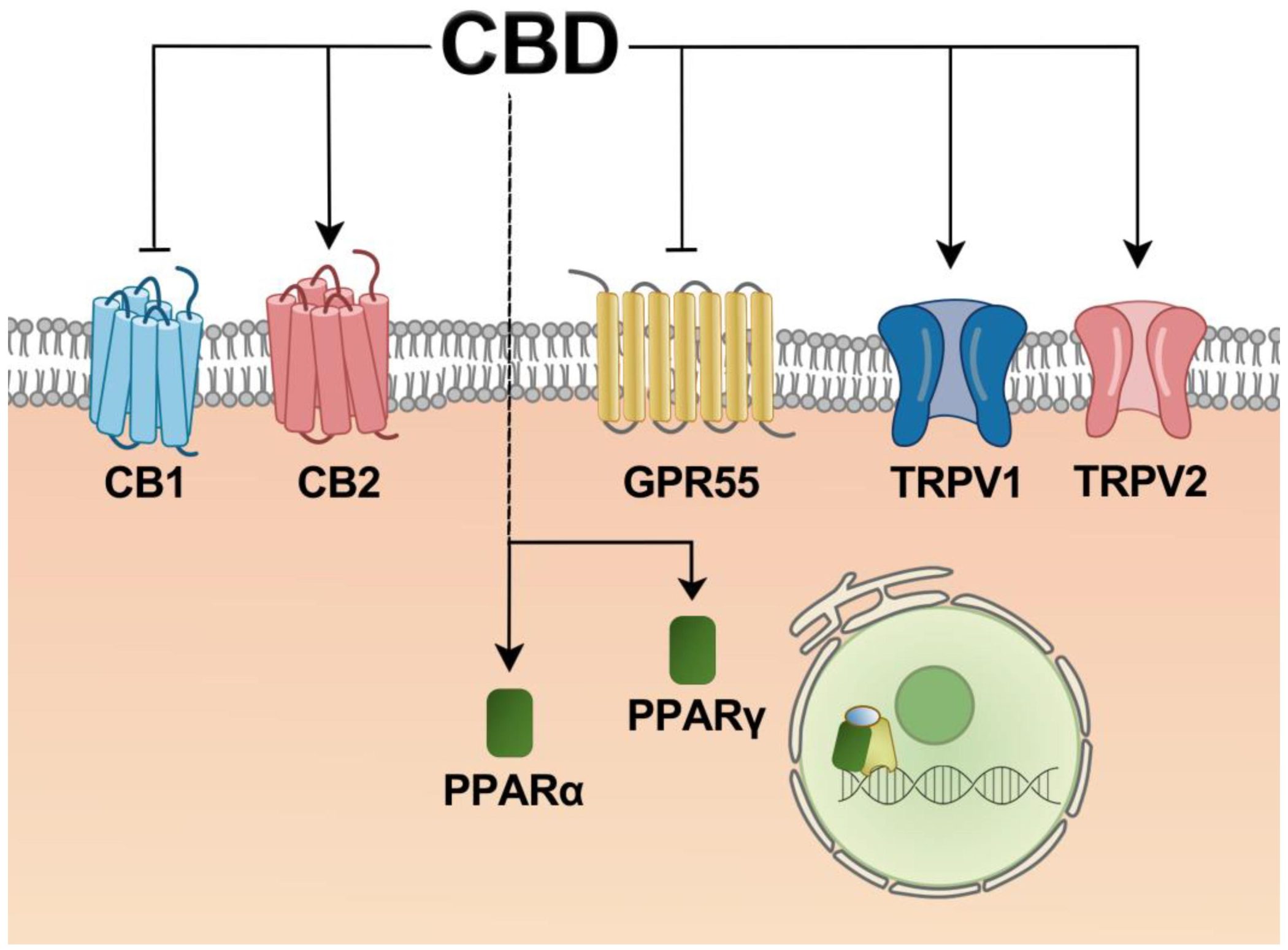
CBD and CBG Are Not the Same
CBD is already widely known. It has been studied in epilepsy, inflammation, anxiety, pain, and a range of other medical areas. CBG is less familiar to the public, but it is becoming increasingly important in cannabinoid research.
CBG is sometimes described as a “minor cannabinoid,” but that phrase can be misleading. Minor does not necessarily mean unimportant. It usually means the compound appears in lower concentrations in the plant compared with major cannabinoids like THC or CBD.
In this study, both CBD and CBG showed benefits, but CBG appeared to have stronger effects on some metabolic markers. Reports on the study noted that CBG more robustly reduced body fat mass, improved insulin sensitivity, lowered total cholesterol, and reduced LDL cholesterol.
That does not mean CBG is ready to become a fatty liver treatment. This was a preclinical study, not a human clinical trial. But it does suggest that CBG deserves far more attention than it has received.
For years, the Cannabis industry has been heavily focused on THC and CBD. Research like this points toward a broader future, where lesser-known cannabinoids may become serious therapeutic candidates in their own right.
Why This Is Important for Cannabis Medicine
The medical Cannabis industry has often suffered from two opposite problems.
On one side, critics dismiss Cannabis as recreational, unserious, or too poorly studied to belong in mainstream medicine. On the other side, some advocates make claims that are far too broad and not supported by enough clinical evidence.
This Israeli study sits in a much better place. It does not claim that Cannabis cures fatty liver disease. It does not suggest that people should start self-medicating with CBD or CBG products. It does something more useful: it identifies a possible mechanism that can now be tested further.
That is how Cannabis medicine has to evolve.
The future will not be built on saying Cannabis helps everything. It will be built on identifying which cannabinoids affect which biological pathways, at which doses, in which patients, and under which clinical conditions.
This study is a good example of that shift. It moves the conversation from general wellness language into serious metabolic pharmacology.
What This Does Not Mean
It is important not to overstate the findings.
This was not a human trial. The results came from animal models. The compounds were administered in controlled conditions, with specific dosing and purity. That is very different from buying a CBD or CBG product online or at a retail store.
It also does not mean smoking Cannabis treats fatty liver disease. The study did not examine smoked Cannabis, THC-rich products, or adult-use consumption. It looked at isolated non-intoxicating cannabinoids in a laboratory model of metabolic disease.
That distinction matters. A medical cannabinoid therapy would need proper formulation, dosing, safety data, clinical trials, and regulatory review. Over-the-counter cannabinoid products vary widely in quality, concentration, and absorption. Many are not designed or tested for serious metabolic disease.
So the responsible interpretation is not that CBD or CBG is now a treatment for fatty liver disease. The responsible interpretation is that these compounds may offer a promising research path.
Why Israel Keeps Leading in Cannabis Science
Israel has been central to modern Cannabis research for decades. Much of that history goes back to the late Professor Raphael Mechoulam, whose work helped define cannabinoid chemistry and the endocannabinoid system.
The Hebrew University has continued to play a major role in this field, particularly in research connecting cannabinoids to metabolism, obesity, liver function, and inflammatory disease.
That scientific culture matters. Cannabis medicine needs more than product development and consumer branding. It needs pharmacology, toxicology, metabolomics, lipidomics, clinical trials, and regulatory-grade evidence.
Israel has been one of the few places where Cannabis has consistently been treated as a serious biomedical platform, not just a consumer category.
The Commercial Implications
If this research eventually translates into humans, the commercial implications could be significant.
Fatty liver disease is a massive global market. It overlaps with obesity, diabetes, cardiovascular risk, and metabolic syndrome. A cannabinoid-based therapy that could reduce liver fat, improve insulin sensitivity, normalize lipid profiles, and restore liver cell function would not be a niche Cannabis product. It would be a serious metabolic drug candidate.
That is where the Cannabis industry may find some of its most important long-term value.
Not in another disposable vape. Not in another lifestyle gummy. Not in another brand fighting for shelf space.
The real opportunity may be in cannabinoid-derived medicines, minor cannabinoid discovery, liver-targeted formulations, synthetic and biosynthetic production, and intellectual property around specific mechanisms of action.
CBD and CBG are especially interesting because they are non-intoxicating. That makes them more plausible candidates for chronic metabolic conditions, where patients may need long-term therapy without impairment.
A More Serious Future for Cannabis
The Israeli fatty liver study is important because it shows what Cannabis research can look like when it is done properly.
The researchers did not simply ask whether Cannabis was “good” or “bad.” They studied specific compounds, in a specific disease model, through specific biological pathways. They measured liver fat, glucose control, lipid profiles, cellular energy buffering, and lysosomal function.
That is the kind of evidence the industry needs more of.
For patients, the promise is still early. Human trials will be needed before anyone can say whether CBD, CBG, or related compounds can meaningfully treat MASLD. But for researchers, investors, and medical Cannabis companies, the direction is clear.
Cannabis is not one medicine. It is a library of compounds.
Some may have little clinical value. Some may be useful only in narrow settings. Others may eventually become the basis for serious therapies in major chronic diseases.
Fatty liver disease may now be one of the most important areas to watch.
Image:Prof. Joseph “Yossi” Tam / Hebrew University
AULV Health is the sponsor of this article series exploring the future of medical Cannabis. The series examines how cannabinoid science is moving beyond traditional conversations around pain, sleep, and anxiety toward deeper questions about inflammation, metabolic dysfunction, healthy aging, and the endocannabinoid system. AULV Health is advancing next-generation metabolic and cannabinoid-based solutions focused on restoring balance across the systems that regulate inflammation, metabolism, and long-term health. Main image: Prof. Yossi Tam, front row, second from left, with members of his research lab at the School of Pharmacy at the Faculty of Medicine of the Hebrew University of Jerusalem. (Courtesy/Tom Barnea)











































